Home MAMMOGRAPHY UPGRADE: INVESTING IN INNOVATION AND COMFORT
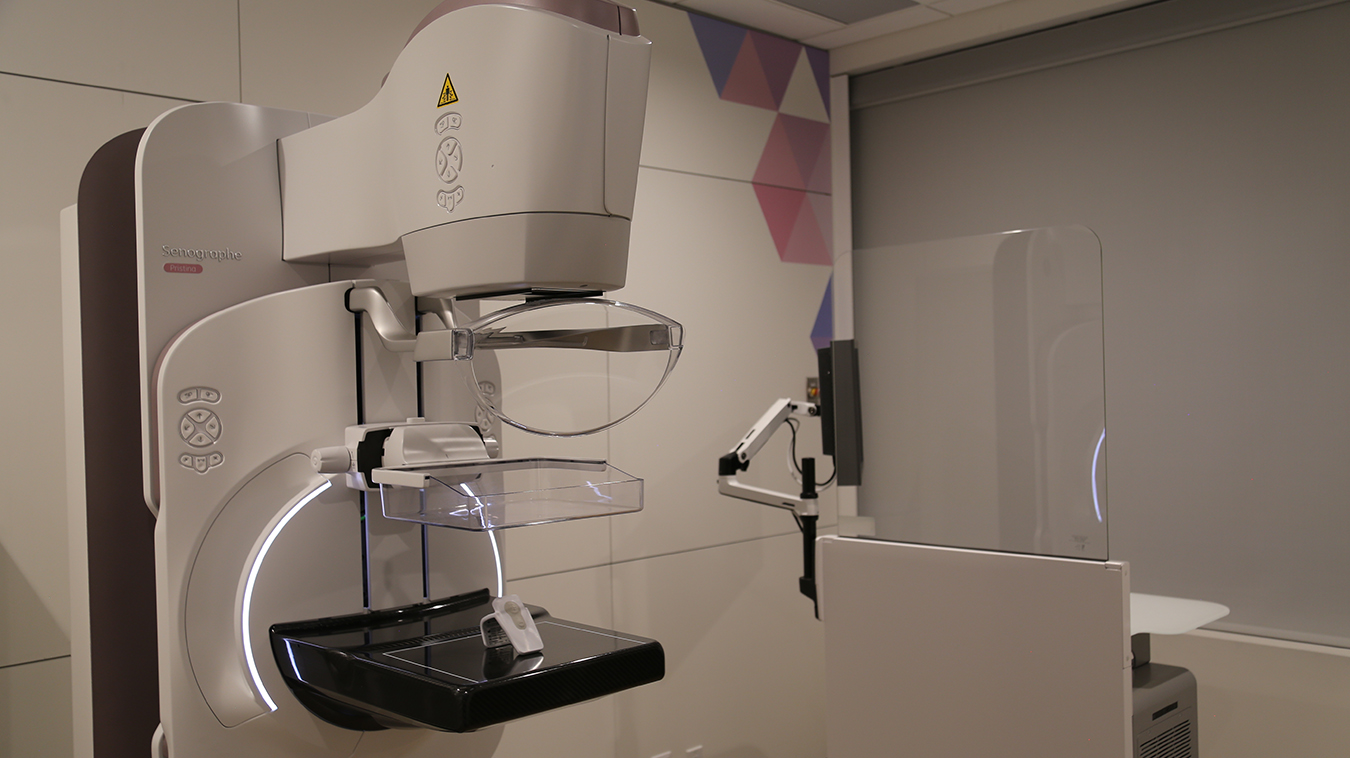
In 2018, Mayfair Diagnostics was the first in Western Canada to install the leading-edge Senographe Pristina Dueta mammography system in two of our clinics. Then, over the next few years, we added this state-of-the-art system to a few more clinics. Now, thanks to a large expansion, we have 11 mammography clinics using the new equipment.
Pristina helps make mammograms more comfortable for patients through its ergonomic design and a special feature called patient-assisted compression. After the breast is properly positioned by a technologist and initial compression is set, you can choose to use a handheld wireless remote control to adjust the level of compression to what’s comfortable for you, under the guidance of a technologist.
Some patients find mammograms uncomfortable, due to the pressure, and are therefore less likely to go for regular breast cancer screening with mammography. Patient-assisted compression allows the patient to reduce the pressure of the exam, while still maintaining excellent diagnostic quality. Giving patients some measure of control during their exam can help decrease their anxiety and increase their willingness to return.
In the four years we have been using Pristina, we have received many positive comments from our patients about their mammography experience:
Since the late 80s, Canada’s breast cancer death rate has been declining thanks to earlier detection from regular mammography screening and improvements in treatment. According to the Canadian Cancer Society, about 87% of women diagnosed with breast cancer are still alive after five years, and the earlier cancer is diagnosed and treated, the better the outcome.
The best way to detect breast cancer early is by having regular screening mammograms before you develop symptoms of breast cancer like pain, lumps, or other changes to the breast. But, many women are reluctant to go for regular screening mammograms because they find the experience uncomfortable.
Having a mammogram every year, or every two years (based on your risk factors), makes it easier for a radiologist to compare your images and see changes or areas of concern. If you wait until you have symptoms, the breast cancer might be bigger and harder to fight.
Mammography is a type of X-ray exam that takes an image of the inside of the breasts.
You will be asked to remove your clothing from the waist up and given a robe. Then your technologist will move you to the correct position between two X-ray plates. At this point, you will have the option to use a handheld remote to adjust the level of compression to what’s comfortable for you, under the supervision of the technologist. This will not affect the accuracy of the images and the technologist will ensure that the optimal level of compression is achieved for the clearest images. Or you can let the technologist control the level of compression.
The surfaces will slowly move together, gently compressing the breast for a short time to minimize your discomfort. Compressing the breast is necessary to get the clearest image of your tissue using the least amount of radiation.
Each breast will be imaged at least twice to create a top and side view for each one. It may be a bit uncomfortable, but it’s very quick, only 10 or 15 minutes in total.
Once the pictures have been taken, one of our doctors will look over them very carefully to check for possible abnormalities or changes compared to previous images. This is the best way to detect breast cancer in its early, most treatable stage, because it provides a detailed look at the internal structure of breast tissue and can reveal changes that are too small to feel.
See what happens during a mammogram.
All women should have a mammogram. Many people start having regular mammograms every year at about age 40, since Alberta Health Care covers one mammogram per year starting at that age. If you have pain or a concern about your breasts earlier than that, you can of course go see your doctor and arrange to have a mammogram. To get a mammogram, you will need to speak to your doctor about your family history, when to start screening, and how frequently you should be screened.
Mayfair Diagnostics recommends screening mammography every year from age 40 to 49, then every two years between age 50 and 75, if there are no risks factors that would necessitate a shorter interval. After age 75, screening frequency will depend on a number of factors, including your medical history.
Across Canada the recommended age to start screening and the recommended screening intervals differ by province. Mayfair’s recommendations for breast screening are aligned with the Canadian Association of Radiologists.
Women with the following risk factors are considered high risk and may be encouraged to start screening earlier and more frequently:
*Dense breast tissue refers to how it appears on the mammogram based on the mix of fatty and fibrous tissue. Women with very dense breasts may require a more personalized screening approach than what is recommended for the general population. This may include both mammography and ultrasound exams.
While the recommendations differ, the ultimate decision rests with women. Understanding the risks and benefits of regular mammogram screening and speaking with your doctor about your medical history is an important first step to decide what’s right for you.
Mayfair Diagnostics has 12 locations which offer mammography exams. However, our Coventry Hills location doesn’t offer patient-assisted compression. Visit our breast imaging page for more information.
Alberta Health Services (2022) “Get Screened.” www.screeningforlife.ca. Accessed April 20, 2022.
Canadian Association of Radiologists (2016) “CAR Practice Guidelines and Technical Standards for Breast Imaging and Intervention.” www.car.ca. Accessed April 20, 2022.
Canadian Cancer Society (2022) “Breast cancer statistics.” www.cancer.ca. Accessed April 20, 2022.
Duffy, S.W., et al. (2020) “Mammography screening reduces rates of advanced and fatal breast cancers: Results in 549,091 women.” Cancer. Accessed April 20, 2022.
Monticciolo, Dr. et al. (2018) “Current Issues in the Overdiagnosis and Overtreatment of Breast Cancer.” American Journal of Roentgenology. February 2018, 210 (2). Accessed April 20, 2022.
We foster a supportive and collaborative culture designed to encourage positive patient experiences and build strong working relationships across the organization:
Our core values shape the way we work with patients, partners, and fellow employees. And, more than anything else, they’re what set Mayfair apart. In everything we do, this is what we strive for:
EXCELLENCE
We share a commitment to high quality and excellence in all that we do. This commitment calls on all of us to achieve the very best of our capabilities and exceed our own expectations.
CURIOSITY
We innovate in everything, from services to processes. We believe meaningful change and effective problem solving come only by looking at challenges and opportunities from new angles and by exercising our creativity and curiosity.
PASSION
We show pride, enthusiasm, and dedication in everything that we do. We are committed to producing and delivering high-quality results and services. We are passionate about our industry and about our company, services, partners, and patients.
COLLABORATION
Our team is supportive of each other’s efforts; we are loyal to one another; and we care for one another both personally and professionally. We promote and support a diverse, yet unified, team. We work together to meet our common goals across Mayfair clinics, locations, and geographies. Only through collaboration on ideas, technologies, and talents can we achieve our mission and vision.
SERVICE
We take pride in delivering exceptional service every day. We listen to every request with an open mind, always looking for opportunities to go above and beyond to create memorable, personalized experiences. We take responsibility to answer our referrers’ and patients’ requests and respect their time by always responding with a sense of urgency.
Start a career with Mayfair Diagnostics — one of Western Canada’s leading medical imaging teams.
Rooted in 100 years of history and headquartered in Calgary, Alberta, we help patients find clarity for their health.
At our clinics in Calgary and area, Regina, and Saskatoon, our team of radiologists, technologists, and support staff work in a truly integrated way to provide exceptional experiences for our patients. Joining our team is more than a job. It’s an investment in your future — a plan for success.
OUR TEAMS
We’re a team of professionals, disciplined in our skills and compassionate with our patients, providing the care and attention they need. At our core, we are a trusted partner in our patients’ health care journey. Our patients, physicians, and other health care providers rely on us for quality imaging to help manage their patient’s health care decisions with certainty. But our business is about more than just imaging. It’s about building lasting relationships and making a meaningful difference in the lives of those we meet.
OUR VISION
A world in which every person has clarity about their health. We push the boundaries of what is possible and embrace change as an opportunity.
We strive to be thought leaders and encourage creativity by providing a safe place for calculated risk taking.
We share best practices across our operations and are recognized by our peers for our work. We engage the best to help propel us forward in achieving our goals.